C. albicans colonies at 30 o on glucose peptone agar are
white or cream, smooth and glistening or occasionally dull and rough,
features which are not really helpful in distinguishing it from other spp.
True hyphae, pseudohyphae and chlamydospores, with clustered blastospores
along the lengths of hyphae, are seen on cornmeal agar.
C. tropicalis is similar (also with true hyphae, but no chlamydospores. There
may also be internodal blastospores. Biochemistry is useful, as C. tropicalis can
ferment sucrose. C. dubliniensis is morphologically and biochemically very similar to C. albicans.
C. krusei doesn't have true hyphae (although the pseudohyphae may
look very hypha-like), with ellipsoidal blastospores.
C. lusitaniae has long pseudohyphae, few branches, prolific small
oval blastospores, and characteristically assimilates rhamnose.
C. parapsilosis has pseudohyphae that often terminate in a swollen
cell, with occasional roundish blastoconidia.
C. glabrata doesn't form pseudohyphae (as noted above), for which
reason it was formerly known as Torulopsis. It has small round to oval
blastoconidia. (C. famata and C. inconspicuosa are similar, as is
Saccharomyces cerevisiae).
}
|
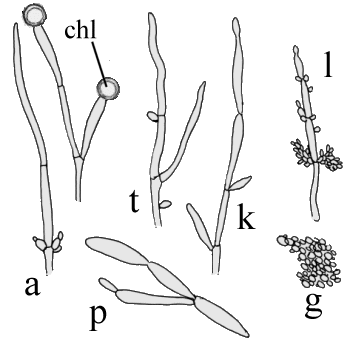
Candida morphology on cornmeal agar
a = albicans, t=tropicalis, k=krusei, l=lusitaniae, g=glabrata, p=parapsilosis; chl=chlamydospore (After Campbell et al.) |
Non-albicans Candidiasis
Not all fungal infections are due to C. albicans - more than a third are due to other organisms such as C. glabrata, C. krusei, C. parapsilosis, C. tropicalis, C. pseudotropicalis, and occasionally very resistant species like C. lusitaniae. In the European SENTRY study, only 53% of 170 episodes of candidaemia were attributable to C. albicans [Diagn Microbiol Infect Dis 1999 Sep;35(1):19-25]. Prominent organisms are:
- C. glabrata (formerly Torulopsis glabrata). Resistance to fluconazole is common, apparently mediated by an "ATP binding cassette transporter gene CgCDR1". Over-the-counter azole antifungals (miconazole, clotrimazole) may promote resistance to fluconazole. The current drug of choice is probably still amphotericin B. Voriconazole appears to be much more effective than fluconazole against C. glabrata. For a review of 139 patients with C. glabrata fungaemia, see [Medicine (Baltimore) 1999 Jul;78(4):220-7]. See also [Clin Microbiol Rev 1999 Jan;12(1):80-96].
- C. krusei is also intrinsically resistant to fluconazole. Here too, voriconazole may be of use. For a recent review of 57 cases of C. krusei fungaemia, see [Arch Intern Med 2000 Sep 25;160(17):2659-64].
- Other fungi: C. parapsilosis infection is becoming more and more important in neonatal ICUs, and the immune compromised. C. tropicalis is not usually a commensal, (unlike C. albicans) ie. isolation suggests infection , and the organism may be fluconazole resistant. C. lusitaniae is interesting (and worrying) as it may be resistant to amphotericin B - surprisingly, fluconazole may work!
Invasive Aspergillosis
| Practical Points |
|
Substantial outbreaks of this disease may occur in immune compromised patients following on inhalation of Aspergillus spores. See for example [Am J Hematol 2001 Apr;66(4):257-62]. In addition, the disorder may be more common than previously thought in patients with chronic obstructive pulmonary disease [Intensive Care Med 2001 Jan;27(1):59-67]! In a Spanish study of AIDS patients, 1.12% had invasive pulmonary aspergillosis - antiretroviral treatment increased survival substantially [Eur J Clin Microbiol Infect Dis 2000 Sep;19(9):688-93].
Invasive aspergillosis (IA) is often fatal. One review reported an overall
fatality rate of 58%, with rates of 87% in bone marrow transplant patients
[Clin Infect Dis 2001 Feb 1;32(3):358-66]. Another review of 595 patients
with probable or confirmed IA showed complete responses to amphotericin B
in only one quarter of patients, with similar high death rates, especially
in the sicker patients who received AB therapy alone, rather than
itraconazole +- AB [Medicine (Baltimore) 2000 Jul;79(4):250-60].
Diagnosis of Systemic Fungal Infection
| Practical Points |
|
The problem with diagnosis and treatment of systemic fungal infection can still often be summed up as "too little too late". Conventional diagnosis of these infections, based on blood cultures or culture of the offending organism from multiple sites, often delays therapy. Patients have frequently been on many different antibiotics for long periods of time in the vain hope that the systemic signs of infection or 'sepsis' will subside. When antifungal therapy is instituted, inappropriate dosing seems quite common.
There is controversy about when you should treat for apparent systemic fungal infections, especially Candida "infection". Most but perhaps not all authors would treat based on isolation of the organism from the bloodstream. There is not even agreement that intravascular lines should be replaced if fungaemia is detected, although most would also regard this as imperative. It has been said that density of infection (some talk about the "colonisation index"), number of positive cultures, isolation from non-contiguous sites, type of organism (C. tropicalis), and isolation from usually sterile fluids all predict the likelihood of severe systemic fungal infection. [Int J Antimicrob Agents 2000 Jul;15(2):83-90]
Candiduria is also controversial, although most would agree that it should be treated once (a) confirmed and (b) risk has been stratified appropriately. This is unfortunately seldom done in clinical practice [Mycoses 1999;42(4):285-9].
Newer tests that have been advocated for early diagnosis of systemic fungal infection include:
- Sandwich ELISA for circulating galactomannan
- Polymerase chain reaction (PCR) shows promise in the diagnosis of Candida infections, even unusual species.
Diagnosis of Invasive Aspergillosis
Invasive aspergillosis may be difficult to diagnose, especially if
one is not aware that it might be present. The presence on high-resolution
CT scan of a "halo" or "crescent air" sign is thought to be diagnostic,
but in one study the crescent sign was only seen
in 10/21 patients [J Comput Assist Tomogr 2001 Mar-Apr;25(2):305-10];
others allege that the halo sign is reliable with early CT, but disappears
later on [J Clin Oncol 2001 Jan 1;19(1):253-259]!
Screening the blood for galactomannan may be very valuable
[Blood 2001 Mar 15;97(6):1604-10] with a sensitivity of up to 90% and specificity
of 98%.
In one prospective study, 14% of 215 patients on chemotherapy appear to have developed
invasive pulmonary aspergillosis [Haematologica 2000 Jul;85(7):745-52].
Polymerase chain reaction may also be of value in early diagnosis
[Br J Haematol 2000 Jan;108(1):132-9].
Antifungal therapy
| Practical Points |
|
We will first discuss the drugs used in treatment, and then treatment of specific fungal infections:
|
|
|
|
|
Amphotericin B
The mainstay of antifungal therapy for severe systemic mycoses is still Amphotericin B (often abbreviated to AB). This predominantly fungicidal agent is available in various forms:- Conventional AB = AB desoxycholate
- Abelcet (AB lipid complex, ABLC).
For a review see [Ann Pharmacother 1997 Oct;31(10):1174-86]. - ABCD = AB colloidal dispersion (Amphocil). This is formulated with sodium cholesteryl sulphate. It appears similar in effectiveness to conventional AB, but with perhaps a slightly better therapeutic index, although big studies are lacking. [Drugs 1998 Sep;56(3):365-83].
- AmBisome = liposomal AB, a small unilamellar liposome preparation (45 to 80nm). This seems to be somewhat less toxic than conventional AB, but is extremely expensive. Efficacy is similar.
Because of the cost of the lipid formulations, and little evidence of increased efficacy (despite better tolerance), most would reserve these for cases where AB desoxycholate is causing severe toxicity. Some have advocated mixing AB in "Intralipid" but the mixture does not appear to be very stable. I would now avoid this practice.
Amphotericin B is useful in treatment of infection with Blastomyces, Coccidioides, Histoplasma, Paraoccidioides, Candida, Cryptococcus, but does have substantial associated toxicity. It is a "polyene", and works on fungi by binding to ergosterol in the fungal cell membrane, disrupting the membrane and killing the fungus. Note that AB appears to have a marked post-antifungal effect (PAFE) of up to ten or more hours, although the clinical relevance of this is controversial. . AB may also have immune stimulatory effects! The drug doesn't work reliably for Trichosporon beigelii, Pseudoallescheria boydii, certain Fusarium spp., and Candida lusitaniae.
Trials of therapy have often been poorly designed, but there is a fair amount of recent evidence that conventional Amphotericin B does work (although you would appear to have to treat 25 patients to save one life), as does liposomal AB. Meta-analyses [Cochrane Database Syst Rev 2000;(4):CD000026] were based on 8 trials showing that IV A/B lowers mortality (RR 0.72, CI 0.51 - 1.02), and three trials of AmBisome. Another analysis [Cochrane Database Syst Rev 2000;(2):CD000026] suggests that routine prophylaxis with antifungals does not influence mortality, a suggestion that few oncologists will happily swallow!
AB's oral bioavailability is under 5%. Systemic (intravenous) administration is associated with a long list of adverse effects, including marked fever (in about 50%), anaphylaxis (about 1 in 100), nausea, vomiting, and nephrotoxicity. Nephrotoxicity includes lowered GFR, increased loss of potassium and magnesium, and even distal renal tubular acidosis. Nephrotoxicity is said to be irreversible if therapy is prolonged [Antimicrob Agent Chemother 1978 13 271-6]. Other nephrotoxic agents may worsen toxicity. It is alleged that nephrotoxicity may be diminished by sodium-loading. Rarely, severe hypertension has been reported in association with AB therapy! The desoxycholate form has a long half life (24-48 hours), and a volume of distribution of about 4 L/kg.
Because it precipitates in normal saline, AB must be mixed in 5% dextrose water, and given via a central line to prevent phlebitis. It is not necessary to adjust dosage in liver failure, but many lower the dose in renal failure(?). The drug is not dialysable. CSF penetration is poor (2-4% of serum levels), but meningeal penetration may be better, and the drug enters the CSF of infants extremely well. We often tend to underdose our patients with (say) 0.5mg/kg - one should probably aim for closer to 1mg/kg or more, especially with more resistant fungi such as Aspergillus. Such doses are achieved with fewer side-effects with newer formulations such as liposomal amphotericin, but the cost is immense. Far higher doses have been used with lipid formulations of AB (even 7mg/kg).
The old tradition of giving a test dose of AB has been questioned,
and some would ignore this approach. (Dose: 1mg in 100ml 5% D/W over 30min).
Conventionally the daily dose is given over about 6 hours, but some
argue that it should be given over a longer period.
Fluconazole and other Azoles
| Practical Points |
|
Azoles (such as fluconazole) inhibit fungal growth by preventing formation of ergosterol, vital for fungal cell membrane integrity. They do this by inhibiting fungal cytochrome P-450 (14-a sterol demethylase), so it is not surprising that these agents have powerful inhibitory effects on some human CYPs. (See our CYP page ). Fluconazole is usually regarded as a "first generation azole", and may well be supplanted in the next few years by newer azoles such as vorizonazole, which have a wider spectrum of activity. Azoles generally have "non-concentration dependent activity" against most fungi.
Fluconazole is mainly used for C. albicans infection (and some other susceptible Candida spp. but NOT C. krusei, and has inconstant activity against C. glabrata). C. albicans may acquire resistance, especially with chronic or recurrent treatment in AIDs patients. Fluconazole may be effective against Cryptococcus neoformans meningitis, and Coccidioidomycosis.
Fluconazole has good GIT absorption, and is renally excreted.
CVVHD causes substantial removal, even more than normal kidneys, and
far greater than with CVVH or intermittent dialysis
[Mycoses 1999 Apr;42(1-2):17-9].
There is a substantial potential for drug interactions owing to inhibition of CYP2C9 ,
and also 3A4.
Volume of distribution may be substantially increased in critically
ill patients.
There is good cerebrospinal fluid penetration.
Adult doses used for severe infections are often in the range of 200mg to 400mg/day, although 800mg/day(+)
has sometimes been used.
Half life (at 200mg/day) is about 27-37 hours, with a V D of 0.7 to 1 L/kg.
{
Susceptibility testing may be of value in
guiding dosing, with the AUC:MIC ratio perhaps a good predictor of
response.
Fluconazole has no post-antifungal effect, unlike AB.
Both human serum and GM-CSF may enhance killing of fungi by fluconazole.
For a review of fluconazole and itraconazole in C. albicans infection see [ J Antimicrob Chemother 2000 Apr;45(4):555]. In neonates, fluconazole has been given at 5 to 6 mg/kg, but long dosing intervals are required in very low birthweight infants [Eur J Med Res 2000 May 23;5(5):203-8].
Details of azoles other than fluconazole are provided below:
Other agents
- itraconazole (capsules poorly bioavailable, elixir better, but far from tasty!; an intravenous form has recently become available. There is complex hepatic excretion. The agent may be an alternative to AB for Aspergillosis, and works for Sporotrichosis, but with treatment of severe disease, blood levels of itraconazole and hydroxyitraconazole are recommended! Pharmacodynamics appear very complex).
- voriconazole {= UK 109,496; Pfizer}
- posaconazole { = Sch 56592; Schering-Plough} - similar to itraconazole, with good Aspergillus fungicidal activity, a really broad-spectrum azole (which may even work against Trypanosoma cruzi)!
- ravuconazole { = BMS-207147; Bristol-Myers Squibb}
- echinocandins (inhibit fungal glucan assembly), preventing fungal
cell wall synthesis; e.g. cilofungin {not currently being used};
V-echinocandin = LY303366 = VER-002 {Eli-Lilly};
MK-0991 = L-743,872 = caspofungin; Have concentration-dependent antifungal
activity, with a substantial post-antifungal effect.
They seem like a fair bet for the future, but need more research -
for example, the combination of V-echinocandin and steroids is lethal in mice.
FK-463, which is echinocandin-like, appears promising. - Flucytosine. Not readily available in many countries, this is mainly used in combination with AB, as otherwise resistance rapidly develops. Gastrointestinal and haematologic toxicity are common.
- in "early development":
- sordarins;
- chitin synthetase inhibitors (polyoxins, nikkomycin Z);
- topoisomerase inhibitors;
- lipopeptides (MK-0991, LY303366, FK463);
- pradimycins (quinones that complex with cell wall mannoproteins of Candida, Cryptococcus and Aspergillus spp). They are toxic and poorly soluble.
- Liposomal nystatin!
Voriconazole
Voriconazole is an azole antifungal. Its plasma protein binding is about 70%, it is mainly cleared by the liver (? CYP 3A4), and has good, rapid oral bioavailability. There is substantial first-pass metabolism, which is saturable. Good for Candida spp, Aspergillus. This includes fluconazole resistant organisms such as C. glabrata. Voriconazole is fungicidal for aspergillus at twice MIC. It is well absorbed orally (about 90%). Voriconazole is also effective against:- Histoplasma, Coccidioides, Blastomyces, Paracoccidioides, Cryptococcus, and dermatophytes;
- Scedosporium apiospermum [Clin Infect Dis 2000 Dec;31(6):1499-501];
- Pseudallescheria boydii [ Clin Infect Dis 2000 Sep;31(3):673-7];
- Penicillium marneffei, Fusarium spp [Mycoses 1999;42 Suppl 2:83-6];
- ? Acremonium strictum [Scand J Infect Dis 2000;32(4):442-4].
It is NOT useful against Sporothrix schenckii and zygomycetes.
Dosage should probably be ~200 to 400 mg/day. In one study,
the loading dose was 6mg/kg BD for 24 hours, followed by 3mg/kg BD.
Side effects include
(reversible) mild-to-moderate visual disturbance in about 14% of
people (enhanced brightness or blurred vision), and raised bilirubin/alkaline
phosphatase in some. Rash occurs in about 4%, and photosensitivity and
erythema have been reported.
Treatment of Systemic Candida Infection
The mainstay of therapy is still amphotericin B, but this may change with
the advent of newer azoles such as voriconazole. C. lusitaniae, which is
often resistant to AB, is fortunately still fairly uncommon. The major
problem is the toxicity of AB, which is substantial. The expense of
lipid formulations of AB practically precludes their use.
Some have advocated the use of fluconazole, often in high doses, for
putative or confirmed Candida infection. The problem with this is that
not only are C. krusei and C. glabrata often resistant to fluconazole,
but with the advent of repeated or long-term fluconazole therapy/prophylaxis (in,
for example, AIDS patients), even C. albicans may be resistant. Dosing
of fluconazole is highly controversial.
Treatment of Invasive Aspergillosis
Amphotericin B is probably still the drug of choice for invasive aspergillosis, although voriconazole may be very effective, and posaconazole has shown promise in experimental models of the disease, as has ravuconazole. Some would even recommend surgical resection for selected cases of invasive pulmonary aspergillosis. A review of 2121 published cases suggests that amphotericin B combined with either rifampicin or flucytosine may be better than amphotericin B monotherapy [Denning DW & Stevens DA: Rev Infect Dis 1990 12(6) 1147-201]. The 'evidence' is not cast in stone.
Treatment of Aspergillus infection in the immune-compromised is urgent , and should be based on clinical or radiological criteria, without waiting for microbiological confirmation.
A fascinating article by Clemons et al. shows that in IL-10 deficient knockout mice, survival after infection with A. fumigatus is better than with wild-type mice that have IL-10. IL-10 promotes a 'Th-2' phenotype, as is seen in asthmatics! [Clin Exp Immunol 2000 Nov;122(2):186-91]
Sequential Therapy
This has become quite popular - initial aggressive amphotericin B therapy may be followed by e.g. long-term fluconazole. This approach is best-documented in cryptococcal meningitis in AIDS patients, but a similar approach (AB followed by itraconazole) has also been used with Aspergillus infection.
Treatment Failures
These are still very common with all systemic mycoses. Often they are thought to reflect the severity of the underlying disease, but there is some concern that more often than not, we underdose our patients with antifungal therapy, use the wrong agents, or start too late. Secondary resistance may also arise. Treatment failure occurs in about twenty to thirty percent of patients with candidaemia, and the death rate in patients is high. In one study of 415 cases of candidaemia, overall mortality was 45%, [CMAJ 1999 Feb 23;160(4):493-9], being lower in children. In invasive aspergillosis, treatment failures are still more common (about 50%).
Secondary resistance is usually seen in more chronic situations, especially in AIDS patients where there is recurrent or prolonged therapy with fluconazole.
Assessment of resistance to antifungal therapy is difficult. The National Committee for Clinical Laboratory Standards (NCCLS) has defined guidelines for testing of azole antifungals, but standards for amphotericin B are not clear. (For details, see Dodds et al.).
For fungal resistance see also [New Horiz 1996 Aug;4(3):338-44]. Primary resistance to fluconazole is common in C. glabrata, and often emerges (or may be primarily present) in C. krusei. C. lusitaniae is primarily resistant to amphotericin, but fortunately, such infections are uncommon.
References
- Dodds ES, et al. Antifungal Pharmacodynamics: Review of the
Literature and Clinical Applications
Pharmacotherapy 2000 Nov;20(11):1335-55.
(A good, current review of a tricky topic - well worth a read) - Harari S. Current Strategies in the Treatment of Invasive
Aspergillus Infections in Immunocompromised Patients
Drugs 1999 Oct;58(4):621-31
(A thorough review of Aspergillosis). - Campbell CK, et al. Identification of Pathogenic Fungi .
PHLS, 1996. ISBN 0 901144 39 8.
(A well-laid out, informative book with superb line drawings of the various fungi. Some of the terminology seems a bit loose). - A
 review of newer antifungals
by Dennis Kim.
review of newer antifungals
by Dennis Kim.
- An
extremely good retrospective from Al-Mohsen and Hughes (1997).
- Candida web-sites:
- The C. albicans server is fairly technical .
- A similar site at Stanford
- www.CandidaPage.com has a host of references of very variable quality.
- Candida web-sites:
| Date of First Publication: 2001-04-11 | Date of Last Update: 2006/10/24 | Web page author: Click here |