Summary of abstractsIt is not the anaesthesiologists decision which patients are operative
candidates. This must be decided by the patient (once given all
possible information), the surgeon, and the doctors who are responsible for
the post operative management of the patient. 1. Preoperative Assessment for Lung Resection. The authors of this valuable article, after a few telling generalisations, get down to the business of reviewing the 'state of the art' in assessing patients for lung resection. They note that perioperative complications are predominantly respiratory, so respiratory assessment is of paramount importance. Initially, one can define a small subset of the population who have normal or near-normal effort tolerance. Such ASA I or II patients do NOT require further respiratory evaluation prior to lung resection. Unfortunately, most patients fall into the larger group where the lung tumour (or other indication for lung resection) is due to smoking that has also exacted its toll on pulmonary function. The authors, despairing of a single test that will predict outcome, fall back on a 'tripod' of assessment criteria:
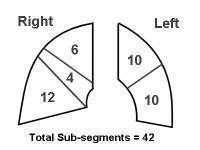
Respiratory MechanicsFor years, predicted post-operative FEV1 has been regarded as a valuable predictor of outcome. To a certain extent, this is still probably valid. The level of predicted post-operative FEV1 that the authors recommend as a 'cut-off' is 40% of normal for that individual. Any patient with a value lower than this 40% of predicted, needs further investigation prior to surgery. (Other possible parameters are the maximum voluntary ventilation, forced vital capacity or even residual volume divided by total lung capacity). A convenient method of prediction of post-operative FEV1 is to estimate the amount of functional lung tissue remaining after surgery based on the number of 'subsegments' in each lobe. The authors' figure 2, sketched below, is useful:
For example, if the preoperative FEV1 is 1.8 litres and a right pneumonectomy is to be done, assuming uniform contributions to FEV1 from all subsegments, the predicted post-operative FEV1 is: FEV1 ppo = (20 / 42) * 1.8 = 0.86 litres, as there will be 20 subsegments left after the 22 subsegments in the right lobe have been removed. The calculations for other predicted post-operative values (such as DLCO and VO 2 max) are similarly calculated. It would seem wise to always relate values to the normal prediction for that individual rather than nominating blanket cut-off values such as a predicted FEV1 of "under 1.0 litres". For practical application of a similar (but not identical) formula, see the paper by Kearney et al (Chest 1994, 105(3) 753-9), where multivariate analysis showed only predicted FEV1 as a significant independent predictor of morbidity. The death rate in this study was an impressively low 1%. Of interest is that in this study age, gender, smoking history, hypercarbia, desaturation on exercise, and preoperative FEV1 under 1 litre were all NOT predictive of outcome. Gas ExchangeThe most useful test of the gas exchange capacity of the lung is the DLCO. A ppoDLCO less than 40% predicted for that patient correlates with increased respiratory and cardiac complications, and is independent of FEV 1 . The traditional values of a PaO 2 of over 60 mmHg and PaCO 2 of under 45 mmHg are questioned as reasonable cut-offs. The authors note that these latter criteria are not absolute contra-indications to surgery, with successful resections now taking place in patients violating the PaO 2 and PaCO 2 criteria, sometimes even combined with lung reduction surgery! Cardio-respiratory reserveAlthough the benchmark for prediction of outcome is still regarded by many as a predicted post-operative maximum VO 2 (VO 2 max), this has been shown to correlate well with patient effort tolerance, notably stair-climbing (3 or more flights of 20 steps/flight at 15 cm/step is acceptable), and the distance walked in 6-minutes (under 650 meters is distinctly poor, correlating with a VO 2 max of under 15 ml/kg). It is suggested (without considerable supporting literature) that the 6-minute walk and exercise oximetry might replace VO 2 max determination. If one adheres to the time-honored gold-standard of VO 2 max, it
is has been claimed that a value under 10 ml/kg/min precludes surgery, and
that with values of over 20 ml/kg/min complications are infrequent.
A systematic review of respiratory functionThe following approach is recommended:-
In addition, the article contains many valuable pointers for the
practising anaesthetist. These include sections on evaluation of other
intercurrent disease, pre-operative optimization (including steroids,
physiotherapy, cessation of smoking and lessening the impact of neoplasms both
locally and systemically), analgesia, and pointers on assessing the ease
of lung isolation which can be obtained from
the pre-operative plain chest film and CT scan.
|
|||||||||||||||||||||||